If you are living with an addiction, I urge you to give up a love that you hate and invite the world into your life.
With descriptions of SMART Recovery, LifeRing, Rational Recovery, Women for Sobriety, 12-Step and alternatives to 12-Step, secular models and spiritual models. Recovery is not a one size fits all process.
My cortex sits atop my brain like my head sits atop my body like the whale rider sits atop the whale. When a destination is reached, the whale rider insists that it was his planned destination all along, and believes it to be so.
At the constitutional level where we work, 90 percent of any decision is emotional. The rational part of us supplies the reasons for supporting our predilections. William O. Douglas, Supreme Court Justice
The pleasure centers of your brain don’t have to control you. Short term thinking does not have to guide your decisions. With motivation and a few simple tools you can take control of your life, honor your values and attain your long term goals.
I am a trained SMART Recovery facilitator, and have been facilitating SMART Recovery meetings since 2010.
A good description of SMART Recovery and some of it’s tools:
I have been in recovery since August 16, 1989 and am interested in helping others overcome their addictions. This first page is devoted to an overview of the site and a short explanation of what steps a person must take to embrace a lasting recovery. More information is available on the following pages:
Reptile Brain? A brief explanation of why this site is called Reptile Dysfunction The Divided Mind How can brains be so stupid? They’re not. That’s the wrong question. Are You Addicted? How to tell if you or someone you care about is addicted. Why Them? An explanation of how smart people can continue making bad decisions. Now What? OK. I’m an addict. So, now what should I do about it? Site Administrator A little about myself and how I got here. Arrival I have broken the cycle of addiction, but how do I stay clean?
—–
How To End An Addiction
- Become aware of the addiction.
- Evaluate how the addiction is affecting your life and decide whether or not you want to end the addiction.
- Learn what’s going on in your brain when you are engaged in the addictive behavior.
- Gain control over the addictive behavior by retraining your brain.
- Learn techniques to avoid relapses.
- Lead a satisfying life to reduce the attractiveness of the addictive behavior.
Become aware of the addiction
If you don’t perceive a problem, there will be no problem to solve. See how the scientific community defines addiction here: 1 and 2 and 3 or 4 or 5
Evaluate how the addiction is affecting your life and decide whether or not you want to end the addiction
You will have to evaluate how the addiction is affecting your life before you will be motivated to change your routines. A good SMART Recovery tool to use for this is the Hierarchy of Values worksheet, where you decide what your true values are and then determine how you are actually spending your time. If you are devoting most of your energies to behaviors which are counter to your values, then you will experience the tension of cognitive dissonance and you can use this tension to motivate you to change. Routines are comforting and safe: we know what to expect from them. What we have become used to doing day after day in the past is a very good predictor of what we will do today. When we change these routines there is a short period of uncomfortableness we must go through before we are at ease again. A good tool for this is the Cost Benefit Analysis (CBA), which can guide you in understanding both what you are getting out of your addiction and the costs and/or risks of the behavior. Read more here: 1 and 2 or 3 or 4 or 5 or 6 or 7
Learn what’s going on in your brain when you are engaged in the addictive behavior.
It is important to understand why addictions can control or radically influence our behavior. People do not choose to destroy or damage their lives and relationships; their behavior is out of control. Once you understand this, you can forgive yourself for the past, embrace a few simple tools to stop the addiction and resist urges, and live a fruitful and healthy life. For a fuller explanation, go here: 1 and 2 or 3 or 4 or 5 or 6
Gain control over the addictive behavior by retraining your brain.
Write out a Cost/Benefit Analysis every day for the first month. It will only take you five or ten minutes. Pick a date around two weeks in the future to actually stop and between now and then, mentally prepare yourself for stopping. Find a peer support group that is compatible with your belief system and makes sense to you. Tell your loved ones and/or friends you are ending your addiction and enlist their support. Make a list of your values and a list of goals you would like to accomplish. If you think an outpatient or inpatient group is indicated and you can afford to attend one, then, by all mean, make arrangements to do so. More on this can be found here: 1 or 2 or 3 or 4 or 5 or 6 or 7
Learn techniques to avoid relapses.
Learn how to interrupt reptile brain commands. You want your logical mind to be running things during this period of your life. Put a rubber band on your wrist and every time you think about the addictive behavior, snap it. If you are still experiencing craving, take 10 long, slow breaths. Promise yourself you will do a Cost/Benefit Analysis before you act on the craving. Read about all the other diversionary techniques which can help here: 1 and 2 or 3 or 4 or 5
Lead a satisfying life to reduce the attractiveness of the addictive behavior.
You want to end this addiction so you and your loved ones can lead a happy, satisfying life. Spend time thinking about what you would like to do in the future. When you become upset or angry, get a handle on your emotions by filling out an ABC. Start leading a life you can be proud of. These things will not happen instantly, but they will not happen at all if you don’t move towards them. Become productive and find people to be with whose company you enjoy. Some ideas can be found here: 1 and 2 or 3 or 4
—–
Please check out the list of 75 Amazing Addiction Recovery Blogs.
—–
What’s the Big Deal?
Why should non-addicts even care about addiction? Why should they be concerned? So some people can’t control their behavior. That’s their problem. Non-addicts shouldn’t have to spend any time or money dealing with problems that others bring upon themselves. Is this even that big of a problem? There has been addiction since we evolved from the apes, and in fact, even before then, for the behavior is evident in members of many other species.
In all honesty, these are fair questions. Let’s try to answer them.
Why should non-addicts care? Well for one thing, because it directly affects them. Drunk drivers kill (100,000 deaths annually ¹ ) and maim others on the road at an alarming rate, and those who are inebriated have lowered impulse control and impaired judgment which sometimes results in antisocial or unpleasant behavior. Smokers have been known to exhale the damn stuff into air we all breathe. Part of the definition of addiction is that addicts will go to extremes in order to keep feeding those habits, resulting in people committing property crimes like theft, shoplifting, fraud and burglaries in order to pay the artificially high prices some of their desired substances may cost. Many addictions cause health problems, which adversely affects our healthcare system. We have decided the way to reduce addictions is to make some addictive behaviors illegal, and so about half of the federal prisoners in the United States, the country with an incarceration rate that is the highest in the world, at 716 per 100,000 of the national population ² , are there for drug crimes. This not only affects addicts negatively, but we all pay for it, even though it does nothing to affect addiction rates ³ .
Is this a big problem? Anne Wilson Schaef points out, in a Huffington Post article, “that some addictions, such as workaholism, are actually applauded in our culture – while others, such as nicotine, TV, internet porn, gambling, and sex addiction, are simply tolerated. But nobody grows up in our country without becoming addicted to something” ¹ . All of us are born with brains which are pre-wired for addiction. Getting scientific information on what percent of the population will become addicted to something at some point in their lives is difficult to attain due to the wide variety of possible addictions, but a conservative estimate would be at least 50% of the population. So, yeah, it’s a big problem. When you look at how much effort we have put into combating terrorism (which has averaged around 74 deaths per year from 1975-2015 ² ) and look at the mayhem caused by addiction, there is no comparison. If you just compare it to the deaths caused only by alcohol and tobacco, you will find that terrorism causes less than .032% of the death due to those two substances. It is, unfortunately, a very BIG problem for all of us.
News From the Field of Addiction:
From HELPGUIDE.org which had “Adapted with permission from the Harvard Mental Health Letter and Overcoming Addiction, a special health report published by Harvard Health Publications”
Understanding Addiction: How Addiction Hijacks the Brain
What Is Addiction?
Key Points
-
-
- Addiction involves craving for something intensely, loss of control over its use, and continuing involvement with it despite adverse consequences.
- Addiction changes the brain, first by subverting the way it registers pleasure and then by corrupting other normal drives such as learning and motivation.
- Although breaking an addiction is tough, it can be done.
-
To get a clear understanding of addiction, please read the full article. Or this article from the NIH.
Or this, from Addictions and Recovery.org:
Brain’s Reward Center
Graphic from Get Real Recovery
Addictive drugs provide a shortcut to the brain’s reward system by flooding the nucleus accumbens with dopamine. The hippocampus lays down memories of this rapid sense of satisfaction, and the amygdala creates a conditioned response to certain stimuli.
To understand what’s going on in the brain as an addiction develops and why addicts find it so hard to end an addiction once it has taken control, please read the whole article.
Judges: Give Defendants A Choice
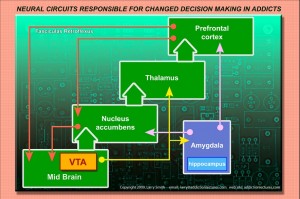
FIGURE 1. Some of the brain structures affected by drugs of abuse. From the following article: Drug addiction: bad habits add up Trevor W. Robbins and Barry J. Everitt Nature 398, 567-570(15 April 1999) doi:10.1038/19208 The mesolimbic dopamine system originates in the ventral tegmental area (VTA) of the midbrain, and projects to the nucleus accumbens (NA). The amygdala (A), hippocampus (HC) and medial prefrontal cortex (PFC) send excitatory projections to the nucleus accumbens. C, caudate nucleus (striatum). FIGURE 2. Labeled “Neural systems of addiction”. From the following article: Drug addiction: bad habits add up Trevor W. Robbins and Barry J. Everitt Nature 398, 567-570(15 April 1999) doi:10.1038/19208 A dopamine-releasing neuron from the ventral tegmental area (VTA) is shown innervating a medium spiny neuron dendritic spine in the nucleus accumbens (NA). The dopamine transporter (DAT) is a main site for cocaine and amphetamine action. These drugs inhibit the re-uptake of dopamine by the VTA neuron, where it is initially produced from the amino acid tyrosine. Dopamine is shown acting at the two main families of dopamine receptor (D1 and D2). These are coupled to guanine-nucleotide-binding proteins (Gsand Gi), components of the intracellular cyclic AMP system, which also includes adenylyl cyclase (AC) and cAMP-dependent protein kinase (PKA). Possible substrates for this kinase include ion channels and the nuclear transcription factors CREB, Fos and Jun. A, amygdala; HC, hippocampus; PFC, prefrontal cortex; EAAR, excitatory amino-acid receptor; Glu, glutamate. (Adapted from ref. 16.)
—–
The video tells us a little about where the current uptick in heroin addiction has come from and also highlights how our perceptions, as a society and a government, concerning who is being affected by this problem determine what we think we should do about it. When I was growing up, heroin addiction was a problem mostly in black and Latino communities. The thinking at the time was “They’re criminals. Put them in prison.” If “they” are overdosing or suffering then it’s not such a big deal, but when “we” and “ours” are in pain, people suddenly become concerned. People are starting to talk about solving problems and helping addicts to move on from their addictions. It’s the same thing that happened during the AIDS epidemic, when government and public opinion concerning what to do about the contagion changed when heterosexuals started getting the disease.
ABC video on the disparity of concern: https://www.youtube.com/watch?v=cskq_zGVSZs
See: The color of heroin addiction — why war then, treatment now?
From SMART Recovery:
The Overcoming Addictions Webcourse is a confidential and interactive web-based course that can help you achieve and maintain abstinence from addictions using SMART’s 4-Point Program. The program has parallel but separate modules for addiction recovery from alcohol, marijuana, opioids, stimulants and compulsive gambling. Details and registration information for this newly released webcourse are available here.
**************************************************************************